Vein disorders are more prevalent than most people know. Millions of adults experience symptoms associated with varicose veins, spider veins, and other venous conditions that impact circulation in the legs. Although these conditions usually start as aesthetic concerns, they can slowly become more serious medical issues that hamper mobility, comfort and overall quality of life. Modern vascular medicine has advanced so that many vein conditions may be treated with safe, minimally invasive procedures. However, one of the biggest questions a patient has before seeing someone about their health is if these services are covered by their health insurance.
This can also help patients understand how individual vein treatments get reviewed by insurance companies. This can depend on a range of factors, including the severity of your symptoms and their medical necessity, diagnostic findings and the specific insurance provider’s policies. Understanding how the insurance systems handle vein care will help patients navigate the system to get the treatment they need.
Cosmetic vs Medical Treatments for Vein Disorders
Dermatology insurance coverage of vein treatment largely depends upon whether the procedure is deemed cosmetic or medically necessary. Cosmetic procedures are usually undertaken to make veins look better, but without an accompanying health risk. Spider vein treatments, for example, are frequently deemed cosmetic because they typically do not produce meaningful medical symptoms.
Medically necessary treatments, on the other hand, correct underlying circulation problems that can lead to complications if ignored. But varicose veins that hurt, swell or change the skin are commonly considered medical conditions instead of cosmetic concerns. Also, insurance is much more likely to cover treatment if these symptoms are documented and valid diagnostic testing conducted.
That distinction is significant because it dictates whether insurance plans would cover the cost of procedures.
Why varicose veins can be a potential medical issue
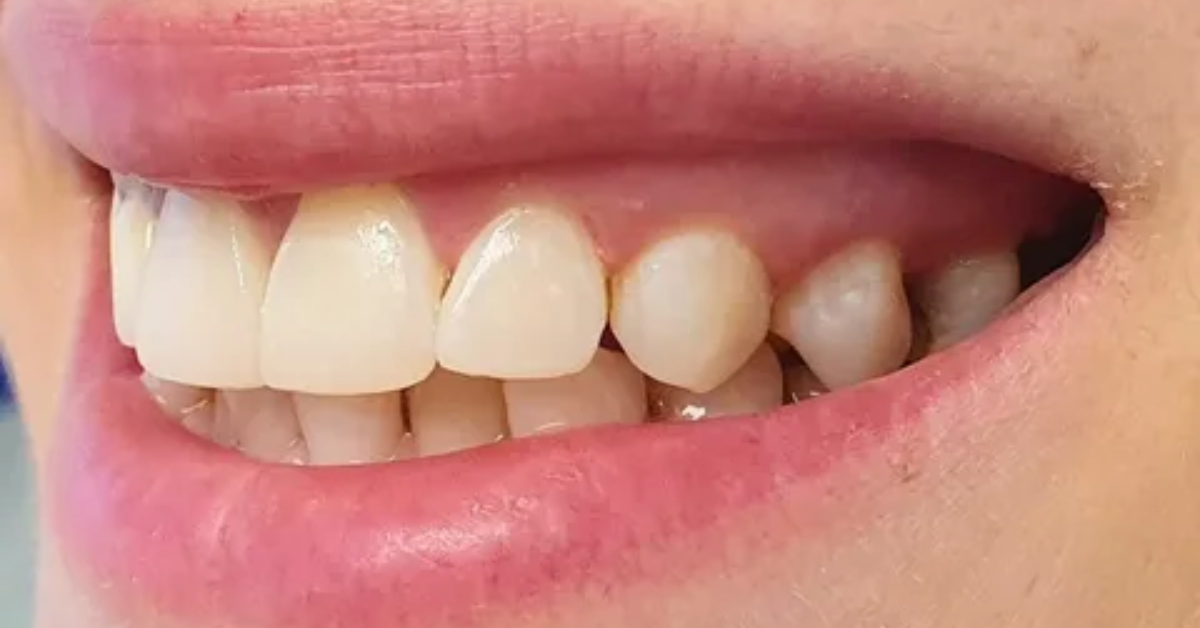
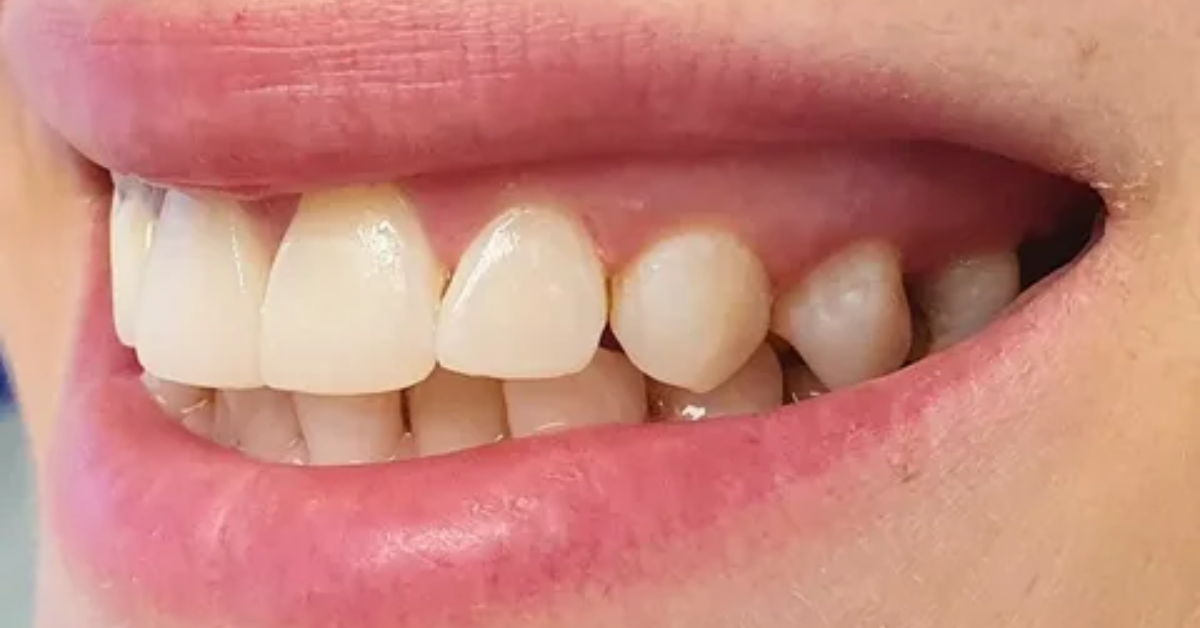
Varicose veins form when the valves in these veins are weakened or damaged. These valves typically aid blood in flowing upward toward the heart, keeping it from pooling in the lower limbs. When they don’t work as they should, blood starts to pool in the veins, causing them to expand and twist underneath the skin.
In the early stages, varicose veins may simply present with mild discomfort or cosmetic-related concerns. In time, though, they can cause more serious symptoms — leg heaviness, aching, swelling and fatigue. In some advanced cases, chronic venous insufficiency can occur that leads to skin discoloration and inflammation and even open sores called venous ulcers.
Because these complications can have a major impact on someone’s health and mobility, many insurance providers acknowledge that there is medical treatment that may need to occur when the symptoms are severe.
Diagnostic Testing and Medical Documentation
Often insurance companies demand proof that vein treatment removes a medical condition before granting coverage. A large part of the process that physicians follow when treating phantom limb syndrome or related conditions is to start with extensive questions involving medical history, symptoms recorded and diagnostic imaging.
Ultrasound imaging is widely used to assess blood flow in the veins and detect dysfunctional valves. This non-invasive test can also indicate if venous reflux exists; the condition where blood is diverted in the opposite direction, away from the heart.
Such tests are conducted, and the documented results submitted to the insurance provider alongside clinical notes detailing their symptoms. This documentation goes to establish that the condition is not merely cosmetic, but is a true medical problem that needs definitive treatment.
Conservative Treatment Requirements
In many instances, in order to qualify for these more advanced procedures, insurance companies require that patients try conservative treatment before they even consider paying. These steps are intended to judge whether symptoms can be controlled without surgical or minimally invasive treatment.
Conservative management usually consists of lifestyle modifications like regular chewing or exercising, leg elevation and use of compression stockings. These over-the-counter, non-medicinal compression garments support vein function by applying gentle pressure that tends to direct other blood flow back toward the heart.
Patients are often told to try these measures for weeks or months before most insurance companies will agree to cover further treatment. If these measures have not worked, doctors may then suggest minimally invasive procedures.
Step 2: Find out More about The Options for Modern Treatment For Vein Disorders.
Newer developments in vascular medicine provide treatment options that help patients effectively manage the underlying condition that leads to painful varicose veins with minimal discomfort. Procedures like endovenous laser therapy and radiofrequency ablation are used in large numbers to effectively close veins gone bad without the need for extensive surgical incisions.
These treatments are typically performed by inserting a thin catheter within the affected vein and delivering controlled energy that leads to collapse and sealing shut of the vein walls. After closure, the body slowly redirects blood flow through healthy veins that are open, resulting in better circulation overall.
Because these surgeries correct a medical issue, rather than just transform one’s appearance, most insurance providers cover them with the appropriate documentation.
Understanding Preauthorization and Insurance Approval
Preauthorization is also a vital part of the insurance process. For many health plans, physicians must first obtain approval from the insurance provider before scheduling a procedure. During this process, medical documentation and diagnostic results are reviewed to assess whether the treatment meets coverage criteria.
Preauthorization helps make sure the procedure is deemed medically necessary based on the patient’s insurance coverage. The process can take some time but prevents financial surprises for patients.
Patients are sometimes aided by healthcare providers and administrative staff, who submit paperwork and communicate with insurers to obtain approval.
Out-of-Pocket Costs and Insurance Plans
And even if insurance coverage is approved, patients may still have to pay certain out-of-pocket costs depending on their specific health plan. Next, deductibles, copayments and coinsurance are standard elements of many insurance policies that dictate patients’ financial contribution to medical services.
Knowing these costs going in may help people plan for the treatment better. Many medical clinics offer financial consultations, or insurance verification services that can give patients an idea of what they might pay before going through with a procedure.
Knowledge of the insurance benefits and limitations empowers patients to take charge of their healthcare.
Accessing Specialized Vein Care
Consulting experienced vascular specialists can greatly influence both treatment outcome and pave the way for quick insurance approval. Vein specialists know how to properly assess venous pathology in order to support and document the medical necessity of treatment.
Those looking for Varicose Vein Treatment in Vineland may find that most clinics offer complete diagnostic services, help with insurance coverage and advanced treatment techniques. Facilities affiliated with the Vein and Vascular Institute collaborate closely with patients to assist them through all the medical and logistical aspects of vein care.
This type of collaborative treatment process is integrated with working through the labyrinths of insurance coverage in order to secure appropriate patient care.
The Importance of Early Evaluation
Seeking medical evaluation early is the single most important way to improve your chances for insurance coverage. Physicians can document the vein issue more accurately and prescribe appropriate remedies if they address vein symptoms before they evolve into serious complications.
Diagnosing the disease early also protects patients from its escalation. Addressing venous disease in the initial stages can relieve discomfort, enhance circulation, and decrease long-term complications.
Patients can adopt proactive measures to safeguard their vascular health by taking symptoms seriously and reaching out to a healthcare professional for medical attention.
Conclusion
While insurance coverage for vein treatments can be sometimes complex, understanding the process gives patients an upper hand to better make informed healthcare decisions. The main determinant of coverage is whether the procedure is deemed medically necessary instead purely cosmetic.
Effective treatment allows many patients to qualify for venous disease procedures supported by their insurance coverage when correct diagnosis and proper documentation are obtained with conservative efforts of treatment. Contemporary minimally invasive treatments have made vein attention safer, more expedient, and available to those users experiencing symptoms.
They can partner with experienced specialists who give their patients an understanding of the terms in their insurance policy and act on that. Overall visibility of internal venous system and its importance is most probably causes more patients to understand that vein treatment is not only an aesthetic issue, but a vital concern for maintaining overall circulatory health and preventing long-term negative effects.